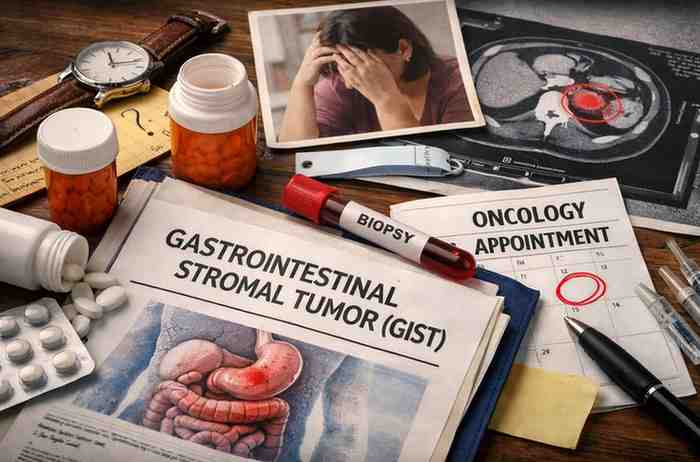
I remember sitting across from a friend whose father had just been told he had a Gastrointestinal Stromal Tumor (GIST).
The doctor had explained it quickly. Medical terms. A few scans. A possible surgery.
But when they left the clinic, the real questions started.
“Is this cancer?”
“Is it curable?”
“Why did nobody notice earlier?”
“Are we already too late?”
And honestly… I’ve now watched enough families go through this to notice something strange.
Most people don’t struggle with the diagnosis itself.
They struggle with the confusing gray zone after it.
Because GIST doesn’t behave like many other cancers.
Not always aggressive. Not always harmless.
Sometimes quiet for years.
And that uncertainty?
That’s where most people feel completely lost.
Over the years—through conversations with patients, caregivers, oncology nurses, and people who’ve lived through treatment—I started noticing patterns.
Mistakes people make early.
Things that scare them unnecessarily.
And a few decisions that quietly change outcomes.
Some of it surprised me.
Some of it honestly made me angry… because patients often learn these things far too late.
First — What a Gastrointestinal Stromal Tumor (GIST) Actually Is
Most people hear “tumor in the stomach” and immediately think of typical stomach cancer.
That’s not what GIST is.
A Gastrointestinal Stromal Tumor (GIST) is a rare tumor that develops from special cells in the digestive tract called interstitial cells of Cajal.
These cells basically act like the pacemakers of digestion, helping muscles move food through the GI tract.
When something goes wrong in these cells—usually genetic mutations like KIT or PDGFRA—they can grow uncontrollably and form tumors.
What surprised me when I started learning about GIST through real cases:
Most of them appear in just a few locations.
Common places doctors find GIST:
-
Stomach (most common)
-
Small intestine
-
Esophagus (rare)
-
Colon or rectum (less common)
And here’s the strange part.
Some people live with a small GIST for years without symptoms.
Others find it only because a scan was done for something completely unrelated.
A kidney stone scan.
Acid reflux tests.
Routine imaging.
That randomness… it throws people off.
The First Emotional Reaction Most People Have
Fear.
But not always for the reason you'd expect.
From what I’ve seen, patients don’t just fear the tumor.
They fear the unknown timeline.
Questions start looping:
-
“Is this fast growing?”
-
“Should we operate immediately?”
-
“Do I need chemotherapy?”
-
“Is this fatal?”
And honestly… the answers vary a lot.
That’s what makes GIST confusing.
Two people with the same diagnosis can have very different experiences.
Why People Usually Discover a GIST Late
I didn’t expect this to be such a common pattern.
GIST tumors often grow quietly.
Many people have no symptoms at all early on.
But when symptoms appear, they usually look like everyday digestive problems.
Things like:
-
Mild stomach discomfort
-
Feeling full quickly
-
Occasional nausea
-
Fatigue from hidden bleeding
-
Black or tarry stools
-
Abdominal swelling
The problem?
Most people dismiss these signs.
I’ve heard versions of the same story over and over.
“Thought it was just gastritis.”
“Doctor said it was probably acid reflux.”
“I ignored it for months.”
And sometimes… it really does look like a harmless issue at first.
The 3 Biggest Mistakes People Make After Diagnosis
Almost everyone I’ve seen struggle with this does at least one of these things early.
1. Assuming all tumors must be removed immediately
Not always.
Small GIST tumors (especially under 2 cm) sometimes get monitored instead of removed.
Doctors may recommend active surveillance.
Which scares patients.
Watching a tumor instead of removing it feels wrong emotionally.
But medically, it can be the safer option in some cases.
2. Thinking surgery alone solves everything
Sometimes it does.
But risk depends on several factors:
-
Tumor size
-
Tumor location
-
Mitotic rate (how fast cells divide)
Two tumors that look similar on scans can behave completely differently.
That’s why pathology results matter so much after surgery.
3. Ignoring genetic mutation testing
This one surprised me.
Mutation testing for KIT or PDGFRA genes often determines whether targeted drugs will work.
Yet many patients don't even know it exists.
And that information can dramatically change treatment decisions.
What Treatment Usually Looks Like in Real Life
From what I’ve seen across different cases, GIST treatment usually falls into three categories.
1. Surgery
For many patients, surgery is the primary treatment.
Doctors try to remove the tumor without rupturing it.
That part is critical.
Tumor rupture can increase the risk of recurrence.
Patients often recover faster than expected after these surgeries.
But emotionally… the waiting after surgery can be brutal.
Because everyone is waiting for the pathology report.
That report determines risk level.
2. Targeted Therapy (Most commonly Imatinib)
This changed GIST treatment dramatically.
Before targeted therapy existed, advanced GIST cases were much harder to control.
Now drugs like imatinib (Gleevec) target the mutations that cause tumor growth.
But here's something people don't expect.
These drugs aren't like traditional chemotherapy.
They're long-term treatments.
Some patients stay on them for years.
3. Monitoring
This is where anxiety spikes.
Patients who undergo monitoring instead of immediate treatment often feel uneasy.
Every scan becomes emotionally charged.
I’ve seen people describe it as “scanxiety.”
Waiting for imaging results can be harder than the treatment itself.
How Long Does It Take to Treat a Gastrointestinal Stromal Tumor?
This question comes up constantly.
The honest answer?
It depends heavily on risk level.
Typical timelines patients experience:
Low-risk tumors:
-
Surgery
-
Periodic scans
-
Often no additional treatment
Intermediate risk:
-
Surgery
-
Possible targeted therapy for 1–3 years
High risk or metastatic:
-
Long-term targeted therapy
-
Ongoing monitoring
Some people live decades after treatment.
That reality surprises many newly diagnosed patients.
What Honestly Surprises Most Patients
Three things consistently shock people.
1. How rare GIST actually is
Many doctors encounter only a few cases per year.
Which means patients often need specialists.
2. How effective targeted therapy can be
Some patients with advanced disease stabilize for years.
3. How emotionally draining monitoring becomes
Even when everything looks stable.
The mental weight of waiting never fully disappears.
Common Questions People Ask (Quick Answers)
Is Gastrointestinal Stromal Tumor (GIST) cancer?
Yes.
It is classified as a type of sarcoma.
But its behavior varies widely.
Some tumors grow very slowly.
Others are aggressive.
What causes GIST?
Most cases involve mutations in the KIT or PDGFRA genes.
These mutations trigger uncontrolled cell growth.
Can GIST spread?
Yes.
The most common spread locations are:
-
Liver
-
Abdominal lining (peritoneum)
However, early-stage tumors often remain localized.
Is GIST curable?
If detected early and completely removed, many cases are effectively cured.
But higher-risk tumors require long-term monitoring.
Objections I Hear All the Time
“If I feel fine, maybe I should wait.”
This is risky.
Small tumors sometimes stay stable.
But large ones can bleed internally without warning.
Medical evaluation matters.
“Targeted therapy sounds scary.”
Understandable.
But many patients tolerate these drugs far better than traditional chemotherapy.
Side effects exist.
But they’re often manageable.
“Rare cancers probably have worse outcomes.”
Interestingly… not always.
Some rare cancers actually respond better to targeted treatments.
GIST is one example.
Reality Check: What Doctors Don’t Always Emphasize Early
A few things patients usually learn later.
Recurrence monitoring is long term
Even after successful surgery.
Follow-up scans may continue for years.
Emotional support matters more than expected
Caregivers often experience stress almost equal to patients.
Not every online story applies
Outcomes vary widely.
Reading extreme cases online can create unnecessary fear.
Practical Takeaways From Watching So Many Cases
If someone close to you receives a Gastrointestinal Stromal Tumor (GIST) diagnosis, these lessons come up repeatedly.
Do this early:
-
Seek a sarcoma specialist
-
Request mutation testing
-
Understand the tumor’s risk classification
Avoid rushing decisions:
-
Not every tumor requires immediate surgery
-
Not every case needs medication
Prepare for the emotional side:
-
Waiting periods are the hardest part
-
Scan results days can be stressful
Focus on patterns that help:
-
Consistent follow-up care
-
Clear communication with specialists
-
Support from patient communities
Most people I’ve watched go through this start in a place of deep fear.
The word tumor does that.
But over time something shifts.
They begin understanding the rhythm of the condition.
The scans.
The treatments.
The waiting.
And strangely… many people settle into a sense of cautious normal life again.
So no — Gastrointestinal Stromal Tumor (GIST) isn’t something anyone wants to hear in a diagnosis.
But it’s also not the hopeless scenario people imagine during those first terrifying days.
I’ve watched enough patients slowly reclaim their routines to know that.
Sometimes the biggest shift isn’t the treatment itself.
It’s learning that life doesn’t stop here.