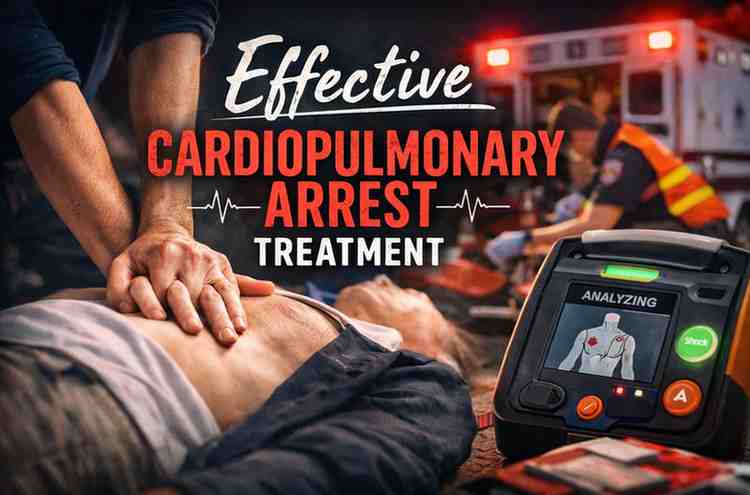
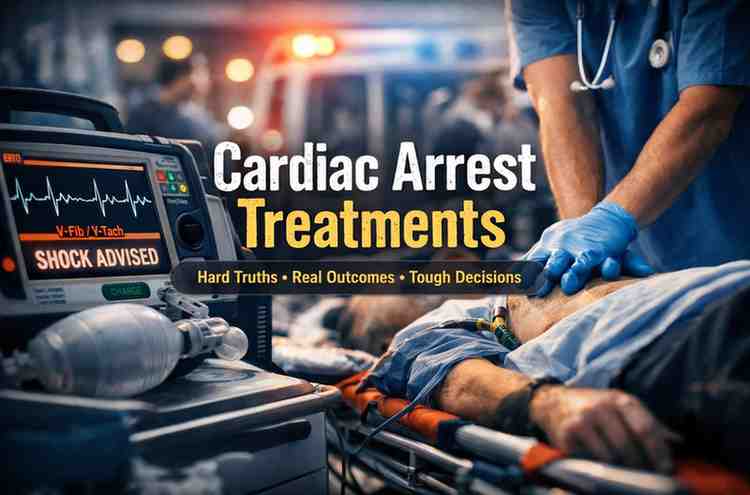
I can’t tell you how many times I’ve watched families freeze in that first minute.
Someone collapses. There’s confusion. Someone says, “Maybe they just fainted.” Another person insists, “Give it a second.” And those seconds stretch.
When people search for Ways to Identify Cardiac Death, they’re usually not curious. They’re scared. Or they’ve already been through something and don’t want to feel that helpless again.
From what I’ve seen—across ER nurses, EMTs, families who’ve lost someone suddenly, and even people who survived cardiac arrest—most people misunderstand what cardiac death actually looks like. It’s not always dramatic. It’s not always loud. Sometimes it’s frighteningly quiet.
Let’s walk through this in a grounded way. Not theory. Not textbook definitions. Real-world patterns.
First, What People Mean by “Cardiac Death”
In everyday language, most people mean sudden cardiac arrest leading to death.
Cardiac death typically happens when:
-
The heart suddenly stops beating effectively
-
Blood stops circulating
-
Oxygen stops reaching the brain
-
Brain injury begins within 4–6 minutes without CPR
Important distinction most people miss:
-
Heart attack = blocked blood flow to the heart muscle
-
Cardiac arrest = electrical malfunction; heart stops pumping
From what I’ve seen, almost everyone uses those interchangeably. That confusion alone delays action.
The Most Reliable Immediate Signs (When It’s Happening Now)
If someone collapses and you’re trying to determine whether this is cardiac arrest (which can quickly lead to cardiac death without intervention), these are the signs that matter most in real life:
1. Sudden Collapse
No warning. No slow slide to the floor.
They were standing. Talking. Walking.
Then down.
This honestly surprises people. They expect clutching the chest first. Sometimes that happens. Sometimes it doesn’t.
2. No Responsiveness
You shake them. You shout their name.
Nothing.
Not groggy. Not confused.
Just… no response.
Most people I’ve worked with mess this up at first. They assume the person is “in deep sleep” or “coming around.” In true cardiac arrest, there’s no meaningful response.
3. No Normal Breathing
This is the one almost everyone gets wrong.
They look for dramatic choking or silence.
Instead, what often happens is agonal breathing — irregular gasping sounds. It looks like they’re trying to breathe.
Families say:
“But they were breathing!”
No. They were gasping.
Agonal breathing is not effective breathing. It’s a brainstem reflex.
If the breathing is:
-
Gasping
-
Snorting
-
Irregular and far apart
Treat it like cardiac arrest.
4. No Pulse (But Don’t Waste Time Searching Forever)
Technically, absence of pulse confirms cardiac arrest.
But here’s the honest truth: untrained people waste critical time trying to find it.
EMTs I’ve spoken to consistently say:
If they’re unresponsive and not breathing normally — start CPR. Don’t debate.
Time matters more than perfection.
What Cardiac Death Looks Like When It’s Already Occurred
Now, if someone has been unresponsive for longer, and death has already occurred, these are the signs medical professionals look for:
-
No pulse
-
No breathing
-
Fixed, dilated pupils
-
Skin turning pale or bluish
-
Cooling of the body
-
Rigor mortis (later stage)
-
Livor mortis (purplish pooling of blood)
But I want to be very clear:
In the U.S., only medical professionals legally declare death in most settings.
Families should call 911 immediately if there’s any doubt.
I’ve seen families hesitate because they’re unsure. That hesitation is something many regret.
What Usually Happens in the First 5 Minutes (Patterns I Keep Seeing)
Here’s what I’ve repeatedly observed from stories:
-
Person collapses.
-
Someone assumes fainting.
-
They wait 30–90 seconds.
-
Panic sets in.
-
Someone searches symptoms on their phone.
-
CPR starts too late — or not at all.
Almost everyone I’ve seen struggle with this does this one thing wrong:
They hesitate because they don’t want to overreact.
In cardiac arrest, overreacting saves lives.
Underreacting costs them.
Early Warning Signs Before Sudden Cardiac Death
Now let’s talk prevention, because most people searching this don’t want to identify death — they want to avoid it.
From what I’ve seen across cardiology consult cases and survivor stories, these patterns show up repeatedly before sudden cardiac events:
Recurring Chest Discomfort
-
Pressure
-
Squeezing
-
Tightness
-
Not always sharp pain
Men tend to ignore it.
Women often describe it as fatigue or pressure.
Unexplained Shortness of Breath
Especially during mild activity.
People dismiss this as aging. Stress. Weight gain.
Sometimes it is.
Sometimes it’s not.
Fainting (Syncope)
This one gets overlooked.
Unexplained fainting — especially during exertion — should never be brushed off.
Heart Palpitations
Racing heart.
Fluttering.
Skipped beats.
Most are benign.
Some are electrical instability warnings.
Severe Fatigue
The kind that feels different.
Heavy. Draining.
Women especially report this before major cardiac events.
I didn’t expect this to be such a common issue until I started hearing the same story over and over.
How Long Does It Take?
If the heart stops completely:
-
Brain injury begins in 4–6 minutes
-
Irreversible damage often begins after 10 minutes without CPR
-
Survival drops dramatically each minute without defibrillation
With immediate CPR + AED use?
Survival rates increase significantly.
The difference between 1 minute and 5 minutes is not small.
It’s everything.
What Actually Improves Survival (Consistently)
From patterns seen across emergency response outcomes:
-
Immediate 911 call
-
Bystander CPR
-
Use of AED within first few minutes
-
Quick EMS response
People assume CPR is complicated.
It’s not.
Push hard.
Push fast.
Center of chest.
100–120 compressions per minute.
I’ve watched people regret not trying more than people regret trying incorrectly.
Common Mistakes That Delay Action
Let’s be blunt here.
These are the repeat offenders:
-
Waiting to see if they “wake up”
-
Misinterpreting gasping as breathing
-
Being afraid of breaking ribs during CPR
-
Searching online instead of acting
-
Assuming young people “can’t have cardiac arrest”
That last one? Dangerous myth.
Sudden cardiac death can happen in:
-
Athletes
-
Young adults
-
People with undiagnosed heart conditions
Rare? Yes.
Impossible? No.
FAQ: Quick, Direct Answers
How can you tell if someone has died from cardiac arrest?
Unresponsiveness, no normal breathing, no pulse. Only medical professionals officially declare death.
Is gasping a sign they’re still alive?
Agonal gasping can occur during cardiac arrest. It is not normal breathing. Start CPR.
Can someone survive cardiac arrest?
Yes — if CPR and defibrillation happen quickly.
Is cardiac death always painful?
Not always. Some people collapse without warning.
Objections I Hear All the Time
“I don’t want to do CPR wrong.”
You probably won’t.
Doing something is almost always better than doing nothing.
“What if they’re just fainting?”
If they’re breathing normally and responsive, it’s likely fainting.
If they’re not responsive and not breathing normally — treat it as cardiac arrest.
“Is it really worth learning CPR?”
Yes.
I’ve seen people save coworkers.
Spouses.
Strangers in parking lots.
The confidence alone changes how people move through the world.
Reality Check: This Isn’t Always Preventable
Here’s where I won’t sugarcoat it.
Even with fast response:
-
Some people don’t survive.
-
Some underlying heart conditions are silent.
-
Some events are catastrophic.
Medicine is powerful.
It’s not omnipotent.
That’s hard to sit with. I know.
Who Should Take This Extra Seriously
-
People with known heart disease
-
Family history of sudden cardiac death
-
High blood pressure
-
Diabetes
-
Smokers
-
Obesity
-
Athletes with fainting episodes
-
Anyone over 40 ignoring recurring symptoms
And honestly?
Anyone living in the United States where heart disease remains a leading cause of death.
Practical Takeaways (If You Want Something Actionable)
Here’s what I tell people plainly:
-
Learn CPR.
A 2-hour class can change outcomes forever. -
Know where AEDs are in your workplace or gym.
-
Don’t ignore chest discomfort that feels “off.”
-
Treat unexplained fainting seriously.
-
If someone collapses and isn’t breathing normally — act immediately.
What to expect emotionally?
Panic.
Adrenaline.
Second-guessing.
That’s normal.
Patience in prevention looks like:
-
Getting regular checkups
-
Not dismissing symptoms
-
Having uncomfortable conversations about family history
It’s not dramatic. It’s boring, actually.
But boring is protective.
Still — none of this makes those moments easy.
I’ve watched people replay those first 60 seconds in their heads for years. Wondering if they missed something. If they should’ve moved faster.
So no — this isn’t magic knowledge that removes risk.
But from what I’ve seen, the people who at least understand the real signs of cardiac arrest don’t freeze the same way. They act faster. They feel less helpless.
And sometimes that shift alone changes the ending.
Sometimes that’s the real win.