Honestly, most people I’ve watched deal with Herpes Simplex Eye Virus never saw it coming.
It usually starts small.
A little eye redness.
Maybe irritation.
Feels like dry eyes or mild conjunctivitis.
One woman I spoke with thought it was just allergy season acting up. A college student assumed it was from staring at screens too long. Another guy kept blaming his contact lenses.
Then suddenly the pain shows up.
Light becomes uncomfortable.
Vision starts feeling… slightly blurry.
And that’s usually the moment people realize something deeper is happening.
By the time the words Herpes Simplex Eye Virus enter the conversation, most people are already frustrated → — sometimes scared. I’ve seen → it happen over and over. The diagnosis sounds dramatic, but the confusing part is this:
The virus itself is incredibly common.
But the eye complications?
Those catch people completely off guard.
And from what I’ve seen across dozens of real cases — the biggest struggle isn’t the virus itself.
It’s misunderstanding how it behaves.
What Herpes Simplex Eye Virus Actually Is (in Plain Language)
That’s not wrong.
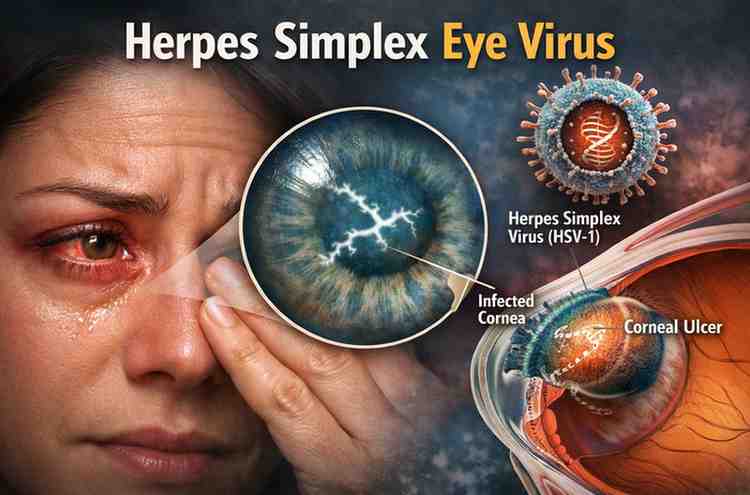
The same virus — HSV-1 — is usually responsible for Herpes Simplex Eye Virus infections.
What changes is where the virus becomes active.
Instead of appearing on the lips, it affects the cornea, the clear front surface of the eye.
Doctors usually call it herpes keratitis.
From what I’ve seen in real cases, the shock for people comes from two things:
-
They didn’t realize herpes could affect the eye
-
They assumed it would behave like a one-time infection
But herpes viruses don’t work like that.
They hide in the nervous system and occasionally reactivate.
That reactivation pattern is where most of the confusion begins.
Why People Usually Miss the Early Signs
The early symptoms are subtle. Almost annoyingly subtle.
And nearly everyone I’ve watched deal with this does the same thing first:
They try to wait it out.
Typical early signs people describe:
-
Mild eye redness
-
Slight watery discharge
-
Sensitivity to light
-
A gritty feeling like something is stuck in the eye
-
Slight blurred vision
The problem?
Those symptoms look almost identical to:
-
Dry eye
-
Allergic conjunctivitis
-
Minor irritation
-
Contact lens problems
One guy I talked to spent five days using over-the-counter eye drops before seeing a doctor.
Another woman kept using allergy drops because spring pollen was high.
By the time they reached an eye specialist, the virus had already started irritating the cornea.
And honestly… this delay is incredibly common.
The Pattern I Keep Seeing With Reactivation
This part surprised me when I first started noticing it.
Many people think herpes eye infections happen once and disappear.
That’s not usually how it plays out.
From what I’ve seen across multiple cases, the virus often follows a pattern:
First infection → quiet phase → random reactivation later
Triggers seem to vary, but the common ones people report include:
-
Stress
-
Illness
-
Fever
-
Sun exposure
-
Eye injuries
-
Fatigue
Sometimes there’s no clear trigger at all.
And that uncertainty is frustrating for people.
One patient told me something that stuck with me:
“It’s the unpredictability that bothers me more than the infection.”
That sentence sums up the emotional side pretty well.
What Actually Happens Inside the Eye
When the virus activates in the eye, it usually targets the cornea.
The virus damages the outer layer of corneal cells.
Eye doctors sometimes see a pattern called a dendritic ulcer — a branching shape on the cornea.
That’s often a clear diagnostic sign.
The reason doctors treat it seriously is simple:
Repeated infections can slowly affect vision if the cornea scars.
Now… here’s the good news most people don’t hear early enough.
Most cases are manageable when treated early.
But the key word is early.
What Usually Works Best (Based on Real Treatment Outcomes)
Almost every case I’ve followed eventually lands on the same medical approach.
Antiviral medication.
Usually one of these:
-
Antiviral eye drops
-
Oral antivirals like acyclovir
-
Sometimes both
And interestingly, many people expect instant improvement.
That expectation causes a lot of unnecessary panic.
From what I’ve observed, the typical timeline looks more like this:
Day 1–3: Symptoms still feel similar
Day 3–7: Pain and redness start improving
Week 2: Most infections stabilize
The biggest emotional shift I notice?
Once people realize the infection is controllable, the anxiety drops dramatically.
Common Mistakes I See People Make
Almost everyone I’ve watched struggle with this does at least one of these things.
1. Waiting Too Long Before Seeing an Eye Doctor
This is the most common mistake.
People assume it's just irritation.
But eye infections escalate faster than people expect.
2. Using Random Eye Drops
Over-the-counter drops can sometimes delay proper diagnosis.
Especially steroid drops.
Steroids can actually make herpes eye infections worse if used incorrectly.
Doctors use steroids sometimes — but very carefully and under supervision.
3. Touching the Eye Too Much
This happens a lot.
People rub their eyes because of irritation →.
That can spread the virus to nearby areas.
4. Stopping Medication Too Early
Symptoms improve, so people stop the antivirals.
Then the infection comes back.
I’ve seen this cycle multiple times.
The Question Almost Everyone Asks
“Is Herpes Simplex Eye Virus Permanent?”
The virus itself stays in the body.
But the eye infection episodes are usually temporary.
Many people go long periods — even years — without another flare-up.
Some people never experience recurrence.
Others have occasional episodes.
It varies widely.
How Long Does Recovery Usually Take?
From the patterns I’ve observed:
Most mild cases improve within 1–2 weeks with treatment.
Vision may take slightly longer to feel normal again.
More severe corneal infections can take several weeks to fully heal.
And honestly…
The emotional recovery sometimes takes longer than the physical one.
People worry about their vision. That’s natural.
Who Should Take This Especially Seriously
Certain groups need faster medical attention.
Including people who:
-
Wear contact lenses frequently
-
Have weakened immune systems
-
Already had herpes eye infections before
-
Experience sudden vision changes
For these people, early treatment makes a huge difference.
People Also Ask
Can Herpes Simplex Eye Virus cause blindness?
Rarely — but repeated untreated infections can damage the cornea.
With early treatment, severe vision loss is uncommon.
Is it contagious?
Direct contact with active herpes lesions can spread the virus.
But routine social contact is not typically a risk.
Good hygiene helps reduce spread.
Can it come back years later?
Yes.
The virus stays dormant in nerves and can reactivate.
Some people never experience another episode.
Others have occasional recurrences.
Does stress trigger eye herpes?
From what many patients report, stress seems to be a common trigger.
It’s not the only cause — but it appears frequently in real cases.
Objections I Hear All the Time
“If the virus stays in the body, what’s the point of treatment?”
Fair question.
Treatment does three things:
-
Stops the current infection
-
Protects the cornea from damage
-
Reduces recurrence risk
Ignoring it simply increases complication risk.
“I feel fine now. Do I still need medication?”
If a doctor prescribed antivirals — yes.
Stopping early is one of the most common reasons infections return.
A Reality Check Most Articles Skip
Herpes Simplex Eye Virus isn’t rare.
But it also isn't a life sentence for your vision.
Still… this part matters.
People who manage it well tend to follow a few consistent habits:
-
They recognize symptoms early
-
They see an eye doctor quickly
-
They finish prescribed medication
-
They avoid rubbing or irritating the eye
Sounds simple.
But honestly?
Most people only learn these lessons after their first scare.
Practical Takeaways I’d Share With Anyone Dealing With This
If someone asked me for real-world advice after seeing all these cases, I’d say:
Take eye symptoms seriously.
Don’t self-diagnose for too long.
Finish antiviral treatments completely.
Even when symptoms improve.
Learn your early warning signs.
People who recognize them early manage recurrences much better.
Reduce eye irritation triggers.
UV exposure, fatigue, and stress seem to play roles in some cases.
Keep follow-up appointments.
Eye doctors monitor the cornea carefully.
Most importantly…
Don’t panic.
The first diagnosis feels overwhelming. Almost everyone I’ve seen go through it feels that wave of fear.
Vision is emotional territory.
But once people understand how the virus behaves — and how manageable it often is — that fear usually settles down.
I didn’t expect this to be such a common story when I first started hearing about it.
People quietly dealing with eye discomfort.
Assuming it's nothing.
Then suddenly learning a virus they associate with cold sores can affect vision.
Still… I’ve also watched something reassuring happen over and over.
Once people understand the pattern — and know how to respond early — the situation stops feeling mysterious.
No, Herpes Simplex Eye Virus isn’t something anyone wants to deal with.
But it’s also not the catastrophic diagnosis many people imagine at first.
And sometimes just understanding that… is the first bit of relief people need. ????️





